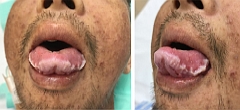
(BMJ)—A 37-yo man w/ no significant PMHx presented w/ a 2-mo hx of generalized fatigue, dysgeusia, and anorexia. He was a plumber and smoked 5 cigarettes per day x17y. Exam: vital signs normal; ammonia odor to breath; white plaque on rim of tongue. Lab tests confirmed the dx. What is it?
|
Uremic stomatitis
|
|
Burning mouth syndrome
|
|
Hairy leukoplakia
|
|
Chronic hyperplastic candidiasis
|
|
Tobacco-associated leukoplakia
|
