Key Points
• Start CPR
• Give O2
• Attach monitor/defibrillator
-
Start CPR1 immediately - Give O2
- Attach monitor/defibrillator
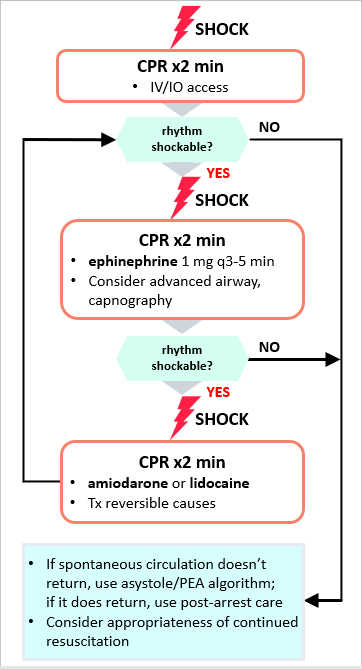
If shockable rhythm (VF/pVT): Defibrillate - Biphasic: Use mfr-recommended energy level (120-200 J), or if unknown, use maximum available; subsequent shocks at same energy level, or consider higher
- Monophasic: 360 J
If shockable rhythm: Defibrillate - Assess rhythm after 2min (5 cycles) of CPR
- Ensure all leads/wires connected
If shockable rhythm: Defibrillate - Assess rhythm after 2min (5 cycles) of CPR
- Ensure all leads/wires connected
Consider amiodarone or lidocaine - amiodarone IV/IO: First dose: 300 mg bolus. Second dose: 150 mg OR
- lidocaine IV/IO: First dose: 1-1.5 mg/kg. Second dose: 0.5-0.75 mg/kg
Treat reversible causes - Hypovolemia
- Hypoxia
- Hydrogen ion (acidosis)
- Hypo/hyper-kalemia
- Hypothermia
- Tension pneumothorax
- Tamponade, cardiac
- Toxins
- Thrombosis, pulmonary
- Thrombosis, coronary
Footnotes 1CPR notes:• Push hard (≥5 cm/2 inches) and fast (100-120/min), allow complete chest recoil
• Minimize interruptions in compressions
• Avoid excessive ventilation
• Change compressor q2min, or sooner if fatigued
• If no advanced airway, 30:2 compression:ventilation ratio
• Quantitative waveform capnography: If PETCO2 <10 mmHg, attempt to improve CPR quality
• Intra-arterial pressure: If relaxation phase (diastolic) pressure <20 mmHg, attempt to improve CPR
2 Advanced airway notes:
• Endotracheal intubation or supraglottic advanced airway
• Waveform capnography or capnometry to confirm/monitor ET tube placement
• Once advanced airway in place, give 1 breath q6sec (10/min) w/ continuous chest compressions -
(1) Start CPR1 immediately - Give O2
- Attach monitor/defibrillator
(2) Evaluate rhythm: If no shockable rhythm – Asystole/PEA - Assess rhythm after 2min (5 cycles) of CPR
- Ensure all leads/wires connected
(3) Resume CPR1 2min - IV/IO access
- Consider advanced airway,2 capnography
(5) Evaluate rhythm: If still no shockable rhythm… - Assess rhythm after 2min (5 cycles) of CPR
- Ensure all leads/wires connected
(7) Treat reversible causes - Hypovolemia
- Hypoxia
- Hydrogen ion (acidosis)
- Hypo/hyper-kalemia
- Hypothermia
- Tension pneumothorax
- Tamponade, cardiac
- Toxins
- Thrombosis, pulmonary
- Thrombosis, coronary
(8) Evaluate rhythm - If no shockable rhythm (Asystole/PEA) and no signs of return of spontaneous circulation (ROSC): Go to (3) or (6)
- If ROSC, go to Post-Cardiac Arrest Care
Footnotes 1CPR notes:• Push hard (≥5 cm/2 inches) and fast (100-120/min), allow complete chest recoil
• Minimize interruptions in compressions
• Avoid excessive ventilation
• Change compressor q2min, or sooner if fatigued
• If no advanced airway, 30:2 compression:ventilation ratio
• Quantitative waveform capnography: If PETCO2 <10 mmHg, attempt to improve CPR quality
• Intra-arterial pressure: If relaxation phase (diastolic) pressure <20 mmHg, attempt to improve CPR
2 Advanced airway notes:
• Endotracheal intubation or supraglottic advanced airway
• Waveform capnography or capnometry to confirm/monitor ET tube placement
• Once advanced airway in place, give 1 breath q6sec (10/min) w/ continuous chest compressions
|
Part 7 & 8: Adult Advanced Cardiovascular Life Support 2015, 2010 AHA Guidelines Update. Circulation. 2015;132:S444-S464; 2010;122:S729-S767.
Epocrates Guideline Synopsis Last Update:
Feb 10, 2021
Source:
AHA
- American Heart Association
Abbreviations
| ACLS |
advanced cardiac life support |
| AHA |
American Heart Association |
| PEA |
pulseless electrical activity |
| PETCO2 |
patient end-tidal carbon dioxide |
| pVT |
pulseless ventricular tachycardia |
| ROSC |
return of spontaneous circulation |
| VF |
ventricular fibrillation |
| VT |
ventricular tachycardia |