-
Suspect Multisystem Inflammatory Syndrome in Children (MIS-C) in any child who presents w/ persistent fever, abdo pain, vomiting, diarrhea, skin rash, mucocutaneous lesions, and in severe cases, w/ hypotension and shock.1 Look for ↑laboratory-confirmed signs of inflammation (esp cardiac markers in majority of pts) and organ dysfxn in setting of recent COVID-19 dz or exposure.1 Most pts (≥65%) progress to shock. All develop organ system dysfxn, incl myocarditis, cardiac dysfxn, and/or acute kidney injury.1 A few develop isolated resp failure2 Be alert for these common sx:3 - Kawasaki-dz like features: conjunctivitis, red eyes, red or swollen hands, feet; rash; red cracked lips, swollen glands
- Toxic shock syndrome-like features w/ hemodynamic instability
- Cytokine storm/macrophage activation or hyperinflammatory features
- Thrombosis, poor heart fxn, diarrhea and GI sx, acute kidney injury
- SOB suggestive of CHF (but resp sx in adults w/ COVID-19 may not show up in pediatric pts w/ MIS-C)
Consider that case definitions continue to evolve:1 - Not all children will have same s/sx
- Some children may have other sx than those listed here
- MIS-C may begin wks after child infected w/ SARS-CoV-2
- Child may be infected from asymptomatic contact; child/caregiver may not be aware of having been infected
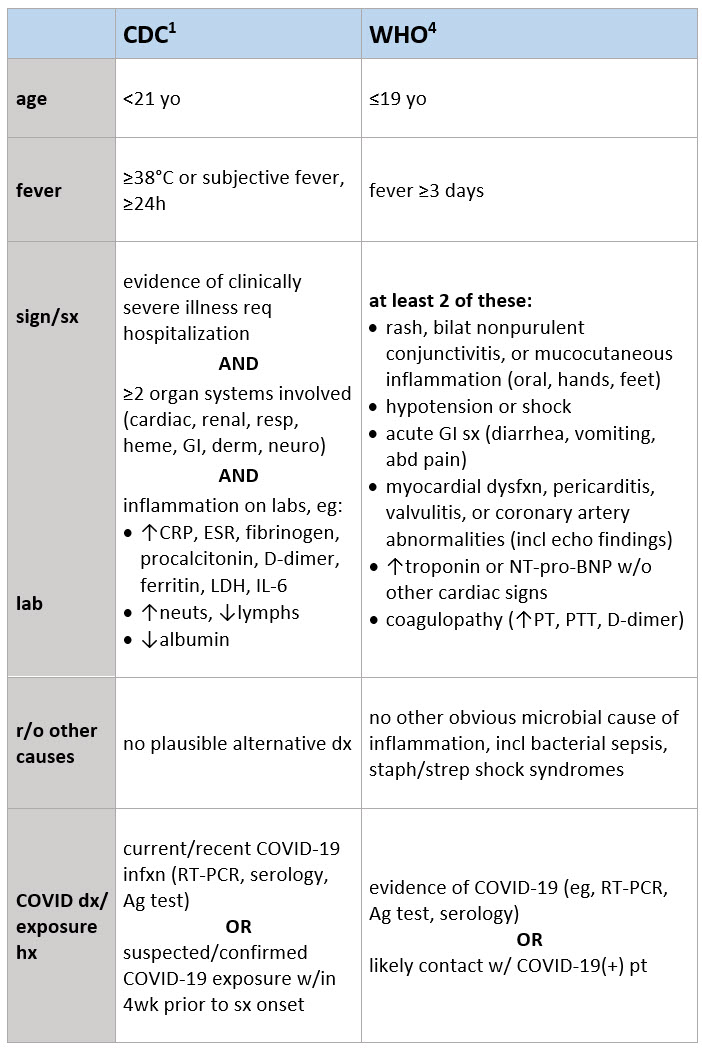
Multisystem Inflammatory Syndrome in Children (MIS-C) Case Definitions Footnotes 1 CDC 2020. Multisystem Inflammatory Syndrome in Children (MIS-C) Associated With Coronavirus Disease 2019 (COVID-19). CDC Health Advisory. May 14, 2020. Accessed 9/21/20
Information for Healthcare Providers About Multisystem Inflammatory Syndrome in Children (MISC-C).
Accessed 9/21/20
2 PIDS 2020. COVID-19 Resources. Pediatric Infectious Diseases Society. Accessed 12/8/20
3 AAP 2020. Multisystem Inflammatory Syndrom in Children (MIS-C) Interim Guidance. Last updated 9/1/2020. Accessed 9/21/20
4 WHO 2020. Freedman S, et al. Multisystem Inflammatory Syndrome in Children and Adolescents Temporally Related to COVID-19. Scientific Brief. May 15, 2020. Accessed 5/29/20 -
Isolate pt & use droplet/contact precautions per local, regional and national standards for COVID-19; consult cardiology, ID, immunology, rheum ASAP; eval for hemodynamic instability, use low threshold for PICU - Use PPE, incl airborne precautions for aerosolizing procedures1
- Monitor cardiopulmonary VS for deterioration continuously; follow std APLS/PALS resuscitation & admit to PICU, if signs of shock1 (≥65% of cases2)
- Obtain cardiac eval early, incl troponin, BNP, EKG, echo; continue serial echo, per PIDS and ACR2,3
- Obtain BCx, start abx per local sepsis protocols1
- Follow inflammatory labs sequentially: CBC, ESR, CRP, PT/PTT, D-dimer, LFTs, cytokines
- Follow RT-PCR, antibodies for SARS-CoV-2; many pts are Ab(+), but RT-PCR(-)2
- Antiviral meds not routine, give only in studies, per RCPCH;1 per PIDS, MIS-C occurs ~4wk after infxn2
- 1st-line tx: IVIG (+/- low-/mod-dose steroids);1,3 can consider high-dose IVIG (1-2 gm/kg) for all; if life-threatening, consider high-dose, IV pulse steroid
- Low-dose aspirin (3-5 mg/kg/day; max 81 mg/day) if: Kawasaki-like features, plt ≥450k or CAA3
- Anticoagulate w/ enoxaparin or warfarin (in addition to aspirin) if large CAA (z-score ≥10.0); enoxaparin alone if dx thrombosis or LVEF <35%3
- Consider anakinra if refractory to IVIG/steroids3
- Enroll in research protocols, incl extra blood specimens before IVIG, immune modulators1,2
- Report cases to local/state health authority4
Footnotes 1 RCPCH 2020. Guidance: Paediatric Multisystem Inflammatory Syndrome Temporally Associated With COVID-19. Royal College of Paediatrics and Child Health. Accessed 5/29/20
2 PIDS 2020. COVID-19 Resources. Pediatric Infectious Diseases Society. Accessed 12/8/20
3 ACR 2020. Clinical Guidance for Pediatric Patients With Multisystem Inflammatory Syndrome in Children (MIS-C) Associated With SARS-CoV-2 and Hyperinflammation in COVID-19. American College of Rheumatology. June 17, 2020. Free full-text PDF
• Serial echo: Repeat at 7-14 days and 4-6wk from presentation, at a minimum. More frequent echo if LV dysfxn or coronary artery aneurysm present. May also consider cardiac MRI 2-6mo after dx if LV dysfxn.
• Perform cardiac CT if distal CAA suspected, but not well-evaluated on echo.
4 CDC 2020. Multisystem Inflammatory Syndrome in Children (MIS-C) Associated With Coronavirus Disease 2019 (COVID-19). CDC Health Advisory. May 14, 2020. Accessed 9/21/20
|